AJOG:事与愿违的分娩方式或致产后抑郁
2015-02-20 Mechront译 MedSci原创
产后抑郁约发生在15%的产妇中,发生率不低,却很容易漏诊。近日Houston KA等人对一项关于分娩方式偏好的纵向研究数据行二次分析,以探究孕妇对阴道分娩的偏好程度以及分娩分式与产后抑郁的联系。研究者们在24-36周询问孕妇其倾向于阴道分娩还是剖宫产,并通过标准的量表对其选择的偏好程度进行测定。然后分别在产后8-10周和6-8月,使用PHQ-9量表,对产妇进行产后抑郁评估。主要结局指标为
产后抑郁约发生在15%的产妇中,发生率不低,却很容易漏诊。
近日Houston KA等人对一项关于分娩方式偏好的纵向研究数据行二次分析,以探究孕妇对阴道分娩的偏好程度以及分娩分式与产后抑郁的联系。研究者们在24-36周询问孕妇其倾向于阴道分娩还是剖宫产,并通过标准的量表对其选择的偏好程度进行测定。然后分别在产后8-10周和6-8月,使用PHQ-9量表,对产妇进行产后抑郁评估。主要结局指标为产后8-10周PHQ-9量表得分。采用多因素回归分析评估孕妇对阴道分娩的偏好程度和最终分娩分式对产后抑郁的影响。其研究成果发表在近期AJOG上。
该研究共纳入160名孕妇,其中33.1%为初产妇,30.6%为前次剖宫产。绝大部分孕妇(92.4%)倾向于阴道分娩,但是其偏好程度跨度较大。按0-1对偏好程度进行自我评估,分越高代表偏好强度越强。在倾向阴道分娩的孕妇中,其偏好强度平均得分为0.658(SD,±0.352)。统计分析后显示,阴道分娩偏好强度和最终分娩方式对产后抑郁评估量表PHQ-9的得分有影响,P=0.047。尤其是,阴道分娩偏好强度越强、最终却经历剖宫产的孕妇,其产后PHQ-9量表得分越高,P=0.027;在最终如愿以偿的经历了阴道分娩的产妇其PHQ-9得分并不高,P=0.761。而阴道分娩强度和最终分娩方式对产后6-8月的PHQ-9量表评分没有显著影响。
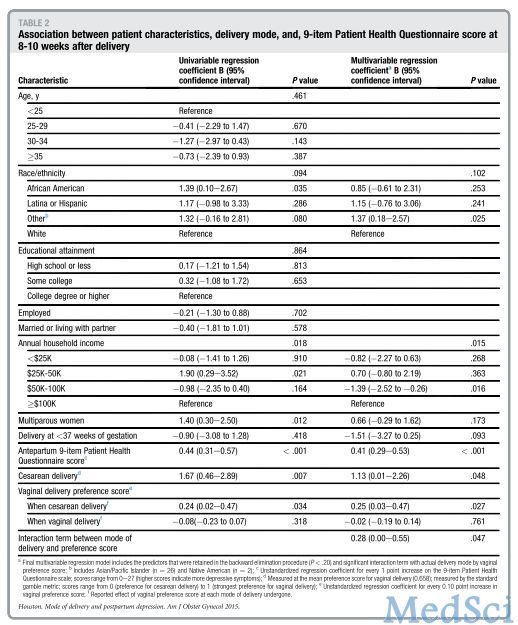
该研究表明,若产前有强烈欲望经阴道分娩,而最终实施了剖宫产的产妇,在产后早期(8-10周)其罹患产后抑郁症的风险增加。
原始出处:
Houston KA, Kaimal AJ, Nakagawa S, et al. Mode of delivery and postpartum
depression: the role of patient preferences. Am J Obstet Gynecol 2015;212:229.e1-7.
下载:
![]() Mode of delivery and postpartum depression the role of patient preferences..pdf
Mode of delivery and postpartum depression the role of patient preferences..pdf
本文是Medsci原创编译整理,欢迎转载!转载请注明来源并附原文链接。谢谢!
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言








#分娩方式#
63
#分娩#
51
#产后抑郁#
55