NEJM:阿奇霉素(azithromycin)并不增加青年和中老年人患者心血管事件死亡
2013-08-15 MedSci MedSci原创
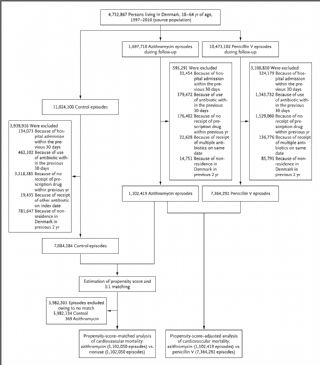
以前研究认为阿齐霉素对心血管高风险人群,能够增加心血管死亡风险。但是在真实世界人群中缺乏研究。为此,一项大规模真实世界中的人群研究,刚刚发表在本期的新英格兰杂志上。这是一项18-64岁丹麦的国家级的历史队列研究,关联处方登记注册数据库,患者死亡原因,以及在1997至2010年间患者的一般情况等资料。评估了使用阿齐霉素达到110万疗程,与未使用抗生素的人群对照(1:1倾向得分匹配),另外,还与736
以前研究认为阿齐霉素对心血管高风险人群,能够增加心血管死亡风险。但是在真实世界人群中缺乏研究。为此,一项大规模真实世界中的人群研究。这是一项18-64岁丹麦的国家级的历史队列研究,关联处方登记注册数据库,患者死亡原因,以及在1997至2010年间患者的一般情况等资料。评估了使用阿齐霉素达到110万疗程,与未使用抗生素的人群对照(1:1倾向得分匹配),另外,还与736万人次使用penicillin V进行对比(也根据倾向得分匹配),观察心血管原因死亡。
结果发现使用阿齐霉素与不使用任何抗生素的人群心血管死亡风险显著增加(RR:2.85, 95CI:1.13 - 7.24).在阿齐霉素组有17例患者死亡,在penicillin V组有146例患者死亡(RR:0.93,95%CI:0.56-1.55)。阿齐霉素并不增加年青人和中老年患者的心血管死亡风险。
原始出处:
Mosholder AD, Mathew J, Alexander JJ, Smith H, Nambiar S.Cardiovascular risks with azithromycin and other antibacterial drugs.N Engl J Med. 2013 May 2;368(18):1665-8.
本网站所有内容来源注明为“梅斯医学”或“MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明来源为“梅斯医学”。其它来源的文章系转载文章,或“梅斯号”自媒体发布的文章,仅系出于传递更多信息之目的,本站仅负责审核内容合规,其内容不代表本站立场,本站不负责内容的准确性和版权。如果存在侵权、或不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言









#中老年#
33
#中老年人#
26
#血管事件#
17
#AZ#
24
#CIN#
23
#MYC#
28